General information about allergy
FamilyWhat is ALLERGY?
Allergy is a reaction of the human defense system against substances which do not commonly cause troubles, and which are normally tolerated by most of the people. When a virus or a bacteria enters the body, this produces defense ANTIBODIES, which destroy the invading agent. In the case of allergy, something similar happens, but antibodies are produced against a normally harmless (pollen, food, …) substance, which is called allergen.
The reaction ALLERGEN-ANTIBODY is responsible for symptoms, which depend on the part of the body where this reaction takes place (coughing, wheezing, sneezing, hives, …) But these symptoms will not appear until the level of antibodies (and hence, the severity of the reaction) exceeds the individual level of tolerance.
Most of allergic people are allergic to several ALLERGENS.
Who is prone to develop allergy?
Allergic diseases are responsible of a large number of medical and labor problems. These diseases use to begin in childhood (although they often do not appear until later in life).
- Food allergy is the most frequent allergy in infants and small children, and they predict the development of allergy to inhaled substances in later life; that is, an infant with allergy to food will very often develop allergy to inhaled allergens when growing to an older age. Likewise, infants who present some diseases at early age (like atopic dermatitis) will often present other allergic diseases when growing (like asthma).
Types of Allergy
Nearly every substance is able to induce allergy in predisposed subjects.
The following links lead to specific pages on the different types of allergy:
- FOOD
- INDOOR ALLERGY (mites)
- OUTDOOS ALLERGY (pollen, molds)
- ALLERGY TO PETS
General recommendations
If your or your child is allergic to one allergen, will probably be allergic to more than one. Nevertheless, you must know that the presence of symptoms depends on the exposure to an amount of allergen able to exceed the tolerance of each patient. For instance, if a patient is allergic to grass pollen, to mites and to dogs, and the recommendations to avoid mites and pollens, this may be enough to remain most of the time below the exposure threshold for presenting symptoms. Therefore, the fact that someone has no apparent symptoms even when having a dog at home does not mean that the patient is not allergic to dogs. It just means that the whole allergenic load is usually below the tolerance threshold; but this may be only transient.
Any case, we must remind that until the patient has not been studied, we can’t know if someone is really allergic, and to what allergens.
Signs and symptoms of Allergy
We come in contact with allergens through the air we breathe, the food we eat, and things we touch. This means that allergic reactions may appear in any part of our body. The most frequent symptoms of allergy are the following:
- Sneezing, often with nose obstruction.
- Coughing.
- Itching of eyes, nose, palate, ears or throat.
- Shiners.
- “Allergic salute” (upwards rubbing of nose, which often gives place to a horizontal groove on the nose).
- Tearing.
- Conjunctivitis (red eyes, eye discharge,…).
- Wheezing, breathing difficulty, chest tightness.
- Skin rashes, hives, itching.
- Stomach pain or cramps, diarrhea, vomiting (mainly in infants and small children).
Allergy and concomitant diseases
Allergy is often more severe than commonly thought. It can affect to a great extent the quality of life of patients. But, even more, allergy can cause or enhance the development of other associated diseases. Consciousness is the key: when someone knows he is allergic and to what allergens, the difference about how to treat and manage allergy and its consequences can be noteworthy.
- Otitis
Otitis (inflammation of the ear) are a cause of frequent visits to the pediatrician, and they are responsible for the highest percentage of causes of hearing loss in children. Recent studies suggest that food allergy may be responsible for repeated episodes of otitis in infants and small children. - Asthma
Asthma is the most frequent chronic disease in childhood, and it affects about 10% of children. The symptoms of asthma are due to bronchial inflammation, which is caused by allergy to house dust mites, pets, molds, pollen, and so on. Identifying and avoiding these allergens will improve symptoms. - Skin rashes
Skin rashes, such as eczema, are very common in infants. They often appear in the first months of life, and they may be caused by allergy to food, like milk or egg. But, furthermore, eczema in a small child must alert about the development of allergy on the long term. About half of the children with eczema will have asthma in the future. Again identifying and controlling the involved allergens will again be the key. - Allergic rhinitis
Rhinitis is an inflammation of the inner layers of the nose, which causes sneezing, itching, obstruction. As with previous diseases, it is essential to find out if it is of allergic nature, and which allergens are involved. - Sinusitis
Nasal and paranasal sinuses are cavities in the skull bones, communicated with the nose through small holes. These can be obstructed by inflammation of the inner layers of the nose, giving rise to sinusitis. Sinusitis (inflammation of sinus) would thus be caused by rhinitis, and the proper treatment of the latter would resolve the former.
Finding the cause
The allergologic study on the possible causes must be performed as soon as the first symptoms suspicious of allergy appear. Newborns rarely present symptoms of allergy. But when milk is started on the diet, some children may present vomiting, diarrhea, infantile colics. Sometimes, when this seems to vanish, skin symptoms (diaper rash, eczema,…) will appear. Later on, “chest colds” or asthma, and finally, allergic symptoms of the nose (rhinitis) or eyes (conjunctivitis) will be evident.
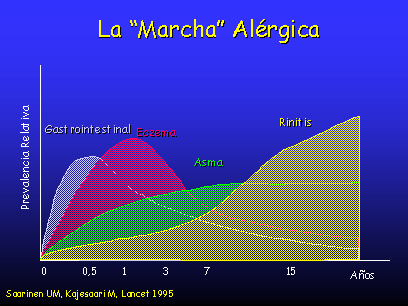
As shown, there is a pattern for the development of allergic diseases: people with allergic predisposition often follow the same clinical course, with changes according to age. This is known as the ALLERGY MARCH.
Hence, finding the cause as early as possible will help stop progression of this march.
Factors contributing to development of allergy.
- Predisposing factors:
- The Atopic Condition. Some people have a genetic predisposition to develop allergic diseases. This predisposition is inheritable. It is more probable that a child is allergic, when other members of the family (mother, father, siblings) are allergic..
- Gender. Some allergic diseases (asthma) are more frequent in boys than in girls.
- Causal factors ➜ ALLERGENS
- Indoor allergens:
- House dust mites
- Molds
- Pets dander
- Cockroaches
- Outdoor allergens
- Molds
- Molds
- Animal dander
- Occupational Allergens ➜ They affect adults who are exposed to some substances because of their jobs (flour in the case of bakers, wood dust in carpenters,…)
- Indoor allergens:
- Coadjuvating and Triggering Factors: These factors do not cause allergy by themselves, but they facilitate that someone becomes allergic to factors described above, or they can trigger symptoms in an already allergic person:
- Air pollution
- Cold air
- Cigarette smoke
- Exercise
- Respiratory infections
Diagnosis of allergy
When your child has any symptoms, you want them to disappear as son as possible. Certainly, itching, conjunctivitis, sneezing or nasal obstruction are not life threatening, but they can become a whole nuisance, and limit the quality of life to a great extent. Again, first of all, to solve this problem, we must find the cause. We must be aware that symptoms of allergic diseases are identical to symptoms of other non allergic diseases.
If you think your child is allergic, you must visit the pediatrician, who, after a detailed clinical history and physical examination, will decide if there is a basis for this suspicion. In this case, the pediatrician will ask for a Allergy specialist to perform the test which will confirm or discard the diagnosis.
Allergy tests
There are two types of tests to find out if a child is allergic:
- Skin prick tests ➜ The skin is punctured with a small lancet through a drop of the suspect allergen. A minute amount of allergen gets into the skin, to see if a reaction occurs. After 15-20 minutes, the presence of a wheal lets know which allergens the patient is sensitized to.
- Blood tests ➜ They are complementary to skin tests. They allow to confirm and to quantify the degree of sensitization. A sample of 2-3 cc of blood is enough to study sensitization to a dozen of different allergens. The Phadiatop® test is a blood qualitative test for the presence of sensitization: a positive result means that the patient will most probably be allergic, while a negative test means the patient will most probably not be allergic. This test is used as a screening method for allergy.
It has been estimated that a person will come in contact during lifetime with thousands of substances capable of inducing allergy.
Fortunately, only a few of them will cause problems. Finding the cause of allergy is sometimes a very difficult task, and the number of tests to be performed for a patient is limited, specially in children. People usually become allergic to substances they have a close and frequent contact with: the more frequent and more intense a contact with a substance, the more probable that one becomes allergic to it. Therefore, the tests to be performed must be based on a detailed medical record, to select the allergens which more probably are involved. For instance, a child with conjunctivitis when near a cat, will probably be sensitized to cat dander. When symptoms appear in Spring, in the countryside, pollen allergy is probable. The specialist must know what are the most relevant plants, molds or mites in the area. Sensitization to pollen of olive tree is very common in the Mediterranean area, while allergy to birch pollen is exceptional. The opposite happens in North Europe countries. House dust mites species may vary according to climate conditions.
On the other side, it is essential to make a correct interpretation of results of tests. Not seldom, a patient may have positive results in tests against some allergens that are not clinically relevant, that is, allergens which are not responsible for triggering symptoms in that patient.
It is important to realize that sometimes symptoms appear when there is a time coincidence of several factors which would not be able to induce those symptoms separately (an amount of allergens together with a viral infection, or exercise, or cigarette smoke, cold air, pollution,…).
This means that the physician who performs, reads and interprets these tests must be a skilled specialist, with the necessary experience and training to reach a accurate diagnosis.
General recommendations for indoor allergen avoidance.
Allergen avoidance mesaures
These measures are intended to avoid as much as posible tose potentially harmful substances found indoors, which can cause asthma and other respiratory and skin symptoms.
GENERAL RECOMMENDATIONS FOR THE WHOLE HOME
These measures are meant to be the ideal condition. As long as they are correctly accomplished, the chances of relapse will decrease. Allergen avoidance is most important in the bedroom, where the child will be at least eight hours a day.
Animal furs and feathers are most allergenic. We must avoid having furred animals (specially cats, dogs and hamsters) and feathered birds at home. If a patient is allergic to them, keeping them may cause symptoms, and if a patient is not still allergic, there is a very high risk to develop allergy to them.
There must be no carpets. There must be no inside flowerpots, as a lot of molds grow on soil. You can keep them outside.
Use plastic washable paints for walls, which must be even and plain. Wall papers must be avoided.
Carry out daily cleaning with a hoover, or washing with water. Use wet cloth for furniture. Do not use a broom or shake dust. Avoid strong odor sprays.
SMOKING IS STRONGLY DISCOURAGED, even if the patient is not at home.
Air-conditioners are useful, if cleaning and maintenance of filters is regularly made.
Every time a patient comes into a house which has long been closed (holidays), thorough cleaning must be made according to these measures.
MITES AVOIDANCE MEASURES:
- For daily cleaning use hoover and wet cloth.
- Replace bed and furniture materials of wool, cotton, fur, feathers by synthetic material.
- Avoid carpets, upholstering, heavy curtains.
- If you are planning to move, choose a dry, sunny place.
MOLDS AVOIDANCE MEASURES:
- Avoid and repair dampness at rooms, kitchen, bathroom.
- Avoid indoor plants, flowerpots, dry flowers.
- Open windows for ventilation of humid, dark romos. Use anti-mold paint.
- Clean filters on air-conditioners and dehumidifiers with anti-mold products.
- Dry clothes and shoes before putting them away.
Measures for bedroom
FEATURES OF ROOM
- When posible, the room must be dry and sunny.
- Use plain wood or tile floor. Avoid carpets.
- Walls must be plain and covered with plastic washable paint. Avoid wall paper or cloth.
- There should be no curtains, or at least they must be made of light synthetic material.
- Avoid unnecessary furniture. If you have a wardrobe, use it only for season clothes, but do not store toys or books.
- Put away clothes into plastic bags.
- Try the child not to use the bedroom as a playroom.
- Avoid upholstering, toys, bookshelves, pictures, posters, furred toys.
FEATURES OF BED:
- The mattress and pillows should preferably be made of foam rubber. Mattress and pillow covers which do not allow the passage of mites are recommended. Alternatively, a plastic protecting sheet may be used. No mattress or pillow with wool, kapok, or feathers should be in the same room.
- Use synthetic blankets. Replace fill-in of feathers by synthetic material.
CLEANING:
- Clean the bedroom every day, with Hoover or water; do not use a broom.
- Expose bed to sun and air, and hoover mattress and pillow daily.
- Clean furniture with a wet cloth. Clean the inside of the wardrobe in the same way daily.
- Once a week, clean walls with a wet cloth, rubbing them downwards.
- Change sheets twice a week, and wash them in hot water. Wash blankets and curtains twice a month.
- Any other bed in the same room must have the same condition. In bunk beds, the allergic child should use the upper bed.
- The regular use of acaricide products is recommended.
